Introduction
Dry eye is a very common condition afflicting more than five million Americans. A lot of people suffer from dry eyes without realizing it. For many decades it was neglected and was sort of a trash bin diagnosis. Even medical doctors were not comfortable handling it. Most just prescribed over-the-counter drops which gave temporary relief really, but did not relieve the condition. Short term measures like taking the red out, propagated a whole industry without alleviating the condition. It's only in the last decade there has been an advancement in management of dry eyes. Technological advancements have generated new diagnostic and treatment modalities. Today management of dry eyes it is a multibillion-dollar industry. To tell you the truth, dry eye is not one condition but many different diseases put together under one terminology, as there was no real treatment until around few years ago.
The reason dry eyes have taken on such a big interest by the industry is because of the realization of importance of tears. The tears are important in the functioning and health of the eye. Lasik causes dry eyes and therefore patients especially above forty may notice a progression of dry eye. Tears are essential for crisp and clear vision. This has been brought to the forefront with presbyopic implants where dry eyes can play havoc with the outcome. That is why people with severe dry eyes like those suffering from Sjogren's syndrome are not good candidates for presbyopia implants. Tears also carry lysozymes which fight bugs so a decrease in tears can lead to susceptibility to infections.
Importance of Tears
Nutrition: The tears bathe the cornea and the conjunctiva cells lining the eye and the lids. In the rest of the body blood vessels and cells of blood provide nutrition and protection. Tears take up that role in the eyes as presence of vessels would obscure vision.
Vision: The air-tear interface is where the tears coating the cornea come in contact with the air in the atmosphere. At this juxtaposition the light changes direction so that it can be further focused by the natural lens.
What Our Patients Say
"Dr. Khanna is an absolute expert. I chose to have PIE surgery and cataract surgery with Dr. Khanna. I only trust him! With PIE surgery I no longer need distance or reading glasses. I have never seen better in MY LIFE!"
"The procedure is very fast and painless. Dr. Khanna and his team were amazing. They worked with my budget and were great at explaining the surgery/prescriptions and recovery time."
Lubrication: The tears form a thin interface between the cornea and the lids to prevent injury to the cornea.
Protection: The lysozymes attack organisms which might try to enter the body through the eyes.
Allergen removal: Everyday a lot of dust and allergens reach our eyes. The tear film entraps them and sends them down the drain into the nose and beyond.
Composition of Tears
The three main components of tear film are Lipid (or the fatty part), Aqueous (or watery part) and Mucin (the rubbery component). These 3 components interact with each other in a complex, physical interaction to produce the tear film. The ratio is as important as the quantity.
The watery component is produced by the main lacrimal gland and some helper or accessory lacrimal glands found in the lids. The lipid component is from the meibomian glands which are located in the cartilage of the lid and open up near the root of the lashes. Mucin is secreted by the small glands called goblet cells, found in the conjunctiva, cornea and the lacrimal gland. Oil floats on water and therefore the lipid and aqueous layer cannot mix. The mucin layer helps the oily layer to mix with the watery layer. Each part plays a specific role and combined their effectiveness is exponential.
There are also minerals, lysozymes and antibodies. Minerals are important for the nutrition of the cornea. Lysozymes and antibodies are the natural defense mechanism of the eye. The proportion and interaction of these three components are as important as the total volume.
The tears are spread across the front surface of the eye by the blinking action of the lids. The eyelids blink around 16 times per minute. The lower lid holds the tear lake. With each blink the lid muscles pump fluid out of various glands, help mix them and produce flow. The upper lid coats the cornea with a thin layer of tear film by its windshield viper action. In a few seconds this film breaks up, to be restored with the next blink.
Production and drainage
The tears are produced by the lacrimal gland located on the upper outer part of the upper lid. They flow across the eyeball to the minute openings in the inner part of the lids. They are joined on this journey by other components secreted from the
glands in the lid margin. The direction of tear flow is due to gravity and shape of eye. It is aided by pumping force generated when lids blink. They then flow down the special tubes to the nose. That is why when you put drops in the eye you may get odd taste in your mouth.
Definition of Dry Eye:
According to the Definition and Classification Subcommittee of the International Dry Eye Workshop, "Dry eye is a multifactorial disease of the ocular surface characterized by a loss of homeostasis of the tear film, and accompanied by ocular symptoms, in which tear film instability and hyperosmolarity, ocular surface inflammation and damage, and neurosensory abnormalities play etiological roles." In simpler terms, dry eye can be defined as when the amount of tears in the eye are not sufficient to carry out the functions attributed to tears. Vision is affected because light is not able to refract at the tear cornea junction. There is a delicate balance between the amount of tears produced, the amount which evaporates into the atmosphere and the amount which is drained through special tubes into the nose. Whenever there is decreased production of tears, an increased evaporation or drainage, or a combination of this, the balance is upset and results in dry eyes.
Symptoms
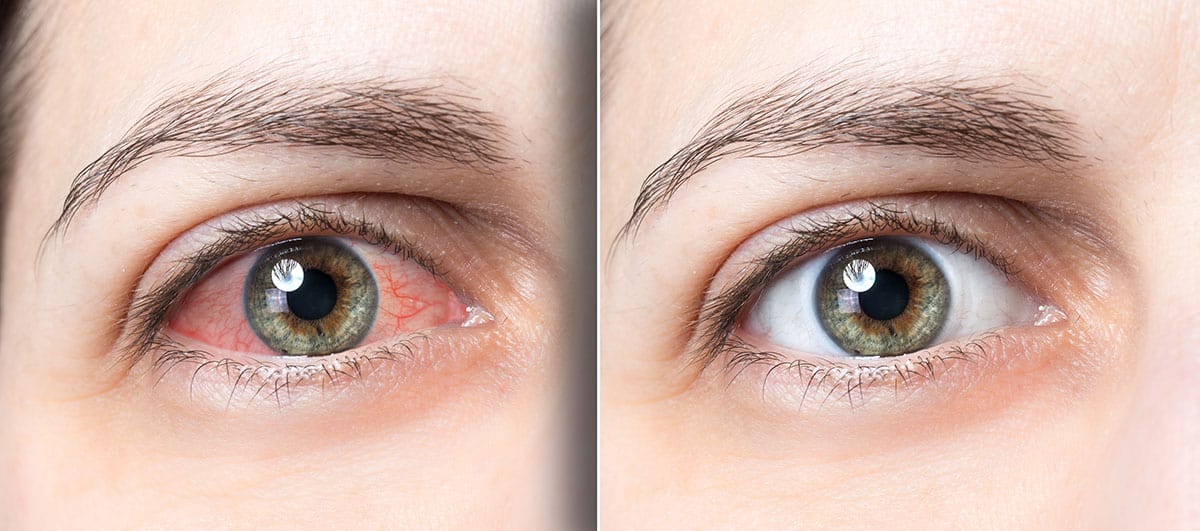
Common symptoms of dry eyes can be easily understood once we have realized the importance of tear film. Tears play the role of blood vessels and blood components, as well as much more. If tears are deficient, the lubrication effect is lost. With each blink, lids scrape the cornea and conjunctiva damaging the top cells. These cells are cast off and rub against the membranes producing the feeling of grittiness. There is also liberation of histamines which causes burning, itching, stinging and light sensitivity. Air and atmospheric temperature stimulate the exposed corneal nerves, producing reflex tearing or watering and pain. Many people wonder how they can have dry eyes if their eyes are watering. There are two kinds of tearing – basal and reflex. Basal tearing is the constant tear production, irrespective of the weather conditions. This production is what's really essential for the nutrition and functioning of the eyes. Reflex tearing is produced in response to external stimuli and is more to wash away allergens.
The lids try to revert the situation by blinking frequently. This can manifest as heavy eyelids and lead to fatigue. As you may have surmised, poor tear film can lead to imperfections in vision, such as blurry or fluctuating vision, interfering with reading, computer vision, watching television, driving, or playing video games. When tears decrease, nutrition to the cornea and conjunctiva is compromised, triggering response mechanisms. Blood vessels dilate and grow larger to bring nutrition and therefore redness is produced from the red blood in the vessels.
When a person dreams, there is rapid eye movement, hence that stage of sleep is termed as REM sleep. In a person with dry eyes, that implies there is more friction between cornea, conjunctiva and the lids. The resultant excess watering overnight can dry up to lead to discharge or even matting of the lids.
Questionnaires
History taking is an art. In the developing field of dry eye, management it is crucial to detect the correct symptoms. To alleviate confusion in terminology and overcome memory lapses, various questionnaires have been developed. They document a patients' subjective dry eye experiences and symptoms to convert them to a more objective and reproducible data set, which can be compared with others or oneself over time. There are numerous questionnaires to assess dry eye patients, but the most popular are the National Eye Institute Visual Function Questionnaire-25 and the Ocular Surface Disease Index.
National Eye Institute Visual Function Questionnaire-25 (NEI-VFQ25)
National Eye Institute came up with this 25-item questionnaire to analyze the irritation from dry eyes and document their effect on activities of daily living and health-related quality of life. The questionnaire analyzes overall health, overall vision, difficulty with near vision, difficulty with distance vision, limitations in social functioning due to vision, role limitations due to vision, dependency on others due to vision, mental health symptoms due to vision, future expectations for vision, driving difficulties, and pain and discomfort around the eyes. Zero is the lowest score while hundred is the highest.
Diagnostic testing
We have seen in the definition that the various causes of dry eye disease result in tear film instability, hyperosmolarity, ocular surface inflammation and damage. It would be prudent to measure these various components to diagnose dry eye disease.
Tear Film Stability is determined by following methods:
Fluorescein TBUT, or Tear Break Up Time: Fluorescein dye is instilled in the eye and the patient is seated at the slit lamp. The patient is asked to blink and the cornea is observed under the cobalt blue light. The time from when the patient blinks until seeing a spot of the cornea that is no longer covered with fluorescein stained tears is counted in seconds. This is the tear break up time. A TBUT greater than 8-10 seconds is usually considered normal, whereas under 5 seconds points to dry eyes.
Non-Invasive TBUT (NITBUT): An image is projected on the cornea. Computer software measures the time to distortion in specific segments of the image.
Ocular Surface Staining
The same fluorescein dye used for TBUT is most commonly applied to detect abnormal or missing epithelial cells. Under the cobalt blue light, gaps in epithelium appear bright green. Lissamine green and rose bengal are two other dyes which detect damaged cells on the conjunctiva. Lissamine green is less toxic and better tolerated than rose bengal.
Tear Volume Assessment
Schirmer's Test: This uncomfortable test is not much used nowadays. A small paper strip is placed over the temporal one-third of the lower lid margin before any drops are instilled. After 5 minutes the length of the strip that is wet is measured. This gives reflex tearing. The test is again performed with anesthetic drops having numbed the eye. This is the basal secretion. Less than 10mm of tear production in 5 minutes, or marked difference between two eyes, is suggestive of dry eye.
Tear Meniscus Assessment: Fluorescein dye under the cobalt blue filter can also detect the tear meniscus. The height above the lower lid can be measured. Anterior segment OCT can also be used to measure the tear meniscus height.
Tear Osmolarity: The painless test utilizes a card mounted on a device and placed over the lower tear meniscus. It can even be used in severe dry eyes as it requires less than 100 nanolitres of tears. Normal osmolarity < 300 mOsm/L in both eyes and a difference between eyes of < 8 mOsm/L.
Matrix Metalloproteinase-9 Test: The tears of patients with dry eyes where their ocular surface barrier function has been compromised have elevated matrix metalloproteinases (MMP). This indicates anti-inflammatory therapy may be beneficial. Allergic conjunctivitis and infection may yield a false positive.
Lactoferrin Test: The protein lactoferrin, produced by the acinar cells of the lacrimal gland, has antimicrobial and anti-inflammatory properties. Dry eye due to decreased aqueous tear production has lower concentrations of lactoferrin.
Meibography: Computerized imaging using black-and-white photography, infrared camera, or near-infrared charge-coupled device (CCD) video camera of an illuminated everted eyelid can outline the silhouette of the meibomian gland. Computer software can do a quantitative analysis of the morphology and structure of meibomian glands.
Interferometry: Lipiview uses interferometry and can be utilized to measure the thickness of the lipid layer.
The Sjo® Test: In the Sjo test, performed to diagnose Sjogren's syndrome, a finger prick sample of blood saturates a specimen filter paper to detect four SS antibodies (anti-SS-A/Ro, anti-SS-B/La, rheumatoid factor [RF], and antinuclear antibody [ANA]) along with three novel, proprietary early biomarkers, antibodies to SP-1, PSP, and CA-6. Anti-SSA antibody is the only serological marker for Sjogren's Syndrome.
Causes of Dry Eyes
Let us consider an example of a swimming pool, where we want an optimum level of water to be always present so we can swim properly. The inlet tap supplies water at a predetermined rate and the drainage regulates the exit of water from the pool. Also, there is evaporation from the surface of the pool. In hot, dry weather, there will be increased evaporation. Whereas on rainy days the water dissipating into the atmosphere will be markedly less. The level of water may decrease in times of drought when there is a restriction on water supply. Finally, if there is a leak in the pool there will be excessive loss leading to lower water level.
Classification of Etiology of Dry Eye Disease
Decreased Production:
- Atrophy of tear producing cells
- Hormone imbalance associated with aging
- Pregnancy
- Thyroid eye conditions
- Diabetes
- Vitamin A deficiency (rare in US)
- Inflammation – Allergies, Eyelid inflammation (blepharitis), Inflammatory eye conditions, including Herpes virus infections and uveitis / iritis
- Suppression by drugs – Medication/supplement use, including psychiatric medicines, OTC cold medicines, anti-histamines, beta-blockers, pain relievers, sleeping pills, diuretics, Hormones replacement, and oral contraceptives
- Congenital absence of lacrimal gland
- Tumors
- Surgical excision of tear producing glands
- Post refractive surgery (LASIK or PRK) – dry eye may generally last three to six months, or longer
- Eye surgery, especially lid surgery such as chalazion removal
- Contact lens use
- Sjogren's syndrome (dry mucous membranes throughout body)
- Other autoimmune disorders including Lupus and/or Rheumatoid Arthritis
- Chemical splashes / injuries to the eyes
Increased Evaporation:
- Air conditioning
- Heat in cold climate
- Outdoor exposure to sun
- Environmental (dusty, windy, hot/dry)
- Infrequent blinking or Poor Blinking, Associated with staring at computer or video screens
- Lid tumors
- Exposure keratitis, in which the eyelids do not close completely during sleep, such as lagophthalmos
- Neurologic conditions, including stroke, Bell's palsy, Parkinson's, trigeminal nerve problem
Increased Drainage:
If the tear punctum is too big than tears may flow down too fast. Rarely there can be an anatomic variation and the tear duct is duplicated. This can again lead to an increased flow.
Incorrect Composition:
The volume is good but there is a mismatch between the oily and water layers. This is the most difficult problem to solve.
Treatment of Dry eyes
Once a clinician knows the cause of the dry eyes, it becomes relatively easier to treat the dryness. The older shotgun approach of throwing artificial tears at everyone benefited some, but did not treat the cause, and even caused harm in a few. Since we have been so diligent in classifying dry eye disease, our treatment modalities will be based on that.
There are some general lifestyle adjustments all people can make before resorting to medications. Eating healthy green vegetables with plenty of water intake is a good first step. Protecting eyes from smoke, dust, wind and sun with a good pair of sunglasses, especially a wraparound type is another easy choice. A wide brimmed cap or hat can increase the protection from these elements.
Exercising regularly, especially in fresh air and decreasing stress through meditation will help reduce systemic diseases and medicines needed to control them. Proper sleeping habits, as well as limiting screen time on computers, tv and phones will also help. Follow the 20/20/2 rule – every 20 minutes look away from your book or screen for 20 seconds and blink 2 times.
Avoid sitting in front of a fan or air conditioner. While driving, have the windows up and point the air conditioning vents away from your eyes. A humidifier at work and while sleeping will moisten the air. Simple humidifiers increase the moisture in dry places and are a more natural and functional way to keep eyes moist. Get enough sleep — about 7 to 8 hours a night.
Increase Production
Foods rich in omega-3 fatty acids have been shown to be of value in improving tear film. Flaxseeds or flaxseed oil, salmon and sardines have high omega 3 content. They are also available as supplements, as well in artificial tears.
Blepharitis, or lid margin inflammation, which progresses to non-infectious inflammation of the lid called chalazion, or even infection of the lid called hordeolum, can be treated by a simple warm compress and lid scrubs. A clean washcloth soaked in warm (not hot) water is applied over the closed eyelids for a few minutes. This may be repeated two or three times.
The warmth allows the oily gland secretions to melt. A thermal pulsation device is an expensive method to accomplish the same goal. Lid scrubs, which are designed for eyes can then be gently rubbed along the base of the eyelashes and lid margin itself to loosen any debris and open the pores.
Lid scrubs are also available as foam which can be applied at the time of shower. Lid scrubs are superior to another method where baby shampoo is rubbed with fingers or Q tips on the base of the lashes.
Drops to reduce eyelid inflammation. Antibiotics may be used alone to tackle any infection present. They are usually combined with steroids for a short time to reduce inflammation which may be preventing various glands from executing their job.
Systemic Antibiotics to improve the quality of tears. An antibiotic known as Doxycycline works with a dual mechanism. It fights any infection present as well as makes gland secretions more liquid. It is administered in a low dose over many weeks. It may cause some bowel disturbances; however, it is otherwise well-tolerated. It should not be given to pregnant women nor teenagers as it can cause discoloration of teeth and bones.
Eyedrops to control inflammation of lacrimal glands. In the last decade there has been commercial development of an immune-suppressing medication cyclosporine (Restasis or Xiidra). This reduces the inflammatory cells in tear glands, especially the lacrimal gland. The suppression of inflammatory cells kickstarts the lacrimal gland again.
Eye drops made from your own blood. They are a last resort when other therapies fail. To generate these eye drops, blood is drawn and centrifuged to remove red blood cells. The remaining liquid is mixed with a salt solution.
Using light therapy and eyelid massage. A technique called 'intense-pulsed light therapy' followed by massage of the eyelids has proven to help people with severe dry eyes.
Acupuncture. Some therapists claim acupuncture therapy can increase tear production.
Decrease Evaporation
Artificial tears – These drops are available with preservatives or without preservatives. Preservatives are added to prevent detonation from external stimuli. They can therefore be packaged in multi-use bottles which can last weeks. These drops can be used one to four times a day. Preservatives are toxic to the epithelium and any further increase in frequency can harm the epithelial cells. Non preservative eye drops on the other hand, have no preservatives and have a limited shelf life. They are packaged as single-use clear vials. They can be put as frequently as every half hour.
Drops vs. Ointments – Lubricating eye ointments are far superior to drops. They adhere and coat the surface of the eyes. They provide longer relief from dry eyes. The eye ointment is thicker and can make vision blurry. They are therefore best used in a small quantity at bedtime. In the morning, water from the shower can be allowed to fall on the closed eyes to wash away excess ointment. Ointments are a good alternative for those who are too busy to put in eye drops. Eye drops can be used at any
time and won't interfere with your vision. This is especially useful for patients who have had recent eye surgery, whose lids open during sleep, or people using Cpap machines.
There is an intermediary product available called gel drops. These are thicker eye drops which last longer.
Eye inserts that work like artificial tears – These inserts, made from hydroxypropyl cellulose (Lacrisert), are inserted daily between the lower eyelid and the eyeball. As they dissolve, they release components similar to eye drops.
Drops that take the red out – These temporary solutions work by constricting the small blood vessels on the surface of the eye. As we have discussed, the blood vessels provide nutrition for the eyes and body. By cutting off this source of nutrition there is more stimulus for blood vessel production. That means over time these very drops cause increased redness.
There are some sunglasses which spray moisture at regular intervals. These eyeglasses also block wind or dust from reaching the eye. Eye covers for sleeping which prevent exposure and evaporation without touching the eye itself. Using special contact lenses called scleral contact lenses protect the surface of the eyes by trapping moisture between the cornea and the lens. They keep the severe dry eye bathed in liquid. Castor oil eye drops may improve symptoms by reducing tear evaporation. This is not a recommended option at present.
| Increase Production | Addition | Prevent Evaporation | Decreased Drainage |
| Oral vitamins | Artificial tears | Sunglasses | Temporary Punctal occluders |
| Warm compresses | Lubricating eye ointment | Wide brim hats | Permananet Punctal occluders |
| Lid scrubs | Humidifiers | Sleeping eye covers | Cautery closure of punctum |
| Drink flax seed oil | Drink water | Surgical closure of punctum | |
| Restasis or Xiidra | Moisture glasses | ||
| Doxycycline | Scleral contact lens | ||
| Autologous serum |

Decrease Drainage
Punctal Occluders – This is an elementary and simple office based painless procedure. The method to decrease the drainage is akin to putting a stopper in the drainage pipe of a spa or a pool. It is customary to start with a temporary punctal occlude in the lower lid. If both eyes are dry it is best to start with only
one lid at a time. The other lid will serve as the control. If there is documented benefit the test can be expanded to the other lid. In the next stage intermediate duration plugs can be inserted. If there is only partial improvement and more is desired the upper punctum can also be occluded. Occluding the upper punctum requires more skill and experience, as gravity tends to pull the occlude out. Everting the upper lid may help in insertion. Similar to the lower lid it is good science to work on one lid at a time starting with temporary one. The reason to start with temporary occluders is that patient can get used to them and if for any reason there is overflow of tears it will resolve quickly. Once mutual satisfaction is established between doctor and patient progression can be made to intermediary or even permanent plugs. We use permanent plugs as a last resort as they are difficult to remove and may serve as a nidus for infection.
Don't worry, in experienced hands this is a quick and pain free procedure requiring only topical anesthesia. The procedure takes a few seconds and can be easily repeated.
There are various types of punctal occluders, or plugs, available as seen in Figure 12.8 below.
| Type | Temporary | Intermediate | Permanent |
| Material | Collagen | Synthetic Polymer | Silicone or Acrylic |
| Duration | 2–4 weeks | 3 -6 months | Lasts for years |
| Usage | Diagnostic | Lasik/ Therapeutic | Therapeutic |
| Dissolution | Dissolves in few weeks | Slowly dissolves over months | Inert |
Heat is applied with a ball cautery. This special instrument has a ball which concentrates heat and transmits to a projection which is inserted into the punctum. Yes, this procedure is only performed under local anesthesia. Radiofrequency controlled needle may also be used.
Surgical Closure
The final option is to do traditional surgery. The patient is put under anesthesia and stiches close the punctum.
Surgery
If the lids are everted, paralyzed or have a tumor, surgical solutions with an oculoplastic surgeon may be considered.
Am I at risk for dry eyes?
You might be more likely to have dry eye if you:
Are age 50 or older
Are female
Wear contact lenses
Don't get enough vitamin A (found in foods like carrots, broccoli, and liver) or omega-3 fatty acids (found in fish, walnuts, and vegetable oils)
Have certain autoimmune conditions, like lupus or Sjögren syndrome
The abive information has been extracted from Rajesh Khanna, MD's book Rejuvenate Aging Eyes.
Choose Hello Treatment at Khanna Vision Institute and Say Bye to Dry Eyes
Experience lasting relief from dry eyes with The Hello Treatment at Khanna Vision Institute. This advanced, customized approach targets the root causes of dry eye syndrome, providing clear, comfortable vision. Led by Dr. Rajesh Khanna, a highly experienced ophthalmologist, the Hello Treatment combines state-of-the-art diagnostics and therapies such as thermal pulsation and Intense Pulsed Light (IPL) to address inflammation and improve tear production. Say goodbye to the discomfort of dryness, redness, and irritation—Hello Treatment is designed for those who want effective, long-term solutions. Book your consultation and start your journey to healthier, hydrated eyes today!
Ready to Transform Your Vision?
Take the first step towards better vision today




